Anesthesia manuals are crucial for standardized protocols, guiding anesthesiologists, residents, and CRNAs through operative scenarios.
The Canadian Anesthesiologists Society (CAS) revised guidelines ensure the highest standards of practice, offering electronic and interactive eBook versions.
Purpose and Scope of Anesthesia Manuals
Anesthesia manuals serve as foundational resources, meticulously outlining best practices for patient safety and optimal outcomes during surgical procedures. Their primary purpose is to standardize anesthetic care, reducing variability and minimizing potential errors across diverse clinical settings. These manuals encompass a broad scope, covering pre-anesthetic assessment, anesthetic techniques – including general and regional approaches – intraoperative monitoring, patient positioning, and comprehensive post-anesthetic care protocols.
The Guidelines to the Practice of Anesthesia, revised by the Canadian Anesthesiologists Society (CAS), exemplify this scope, reserving the right to control publication and distribution. They aim to guide practitioners through all operative scenarios, ensuring adherence to the highest standards. Modern manuals increasingly integrate electronic resources, featuring links to procedures and bundled interactive eBook editions accessible on various devices. Furthermore, educational series, including expert-led webinars and seminars, support the practical implementation of these guidelines, bridging the gap between theory and real-world application for safe and effective anesthetic practice.
Importance of Standardized Protocols
Standardized protocols within anesthesia manuals are paramount for enhancing patient safety and optimizing clinical workflows. They minimize ambiguity, ensuring all members of the operating room team adhere to consistent, evidence-based practices. This consistency is particularly vital during complex surgical procedures where rapid decision-making and coordinated action are essential. The Guidelines to the Practice of Anesthesia, developed by the Canadian Anesthesiologists Society (CAS), underscore this importance by providing a framework for consistent care.
Such protocols reduce the risk of preventable complications, improve communication, and facilitate efficient resource utilization. They also serve as valuable tools for training and education, enabling anesthesiologists, residents, and CRNAs to develop and maintain proficiency in anesthetic techniques. The integration of electronic resources, like linked procedures within the manuals, further supports adherence to these standards. Ultimately, standardized protocols, as championed by organizations like CAS, contribute to a culture of safety and continuous improvement within the field of anesthesia.
II. Pre-Anesthetic Assessment and Preparation
Pre-anesthetic assessment involves a thorough patient history, physical examination, and laboratory investigations.
Airway assessment and management planning are critical steps for safe anesthesia delivery.
Patient History and Physical Examination
A comprehensive patient history is the cornerstone of pre-anesthetic assessment, demanding meticulous attention to detail. This includes documenting pre-existing medical conditions – cardiovascular, respiratory, neurological, endocrine, and renal – alongside current medications, allergies (including latex), and prior anesthetic experiences, noting any adverse reactions.
Specifically, inquire about difficult intubation history, obstructive sleep apnea, and bleeding disorders. A detailed surgical history, including the nature of the planned procedure and its anticipated duration, is also essential.
The physical examination should focus on assessing airway patency – Mallampati score, thyromental distance, and neck mobility – alongside cardiovascular and respiratory status. Auscultate heart and lung sounds, evaluate blood pressure and heart rate, and assess for signs of congestive heart failure or pulmonary disease. Neurological assessment should include a brief mental status examination and assessment of peripheral nerve function.
Documenting these findings accurately is paramount for formulating a safe and effective anesthetic plan tailored to the individual patient’s needs and risk profile.
Pre-operative Laboratory Investigations
Pre-operative laboratory investigations are guided by patient history, physical examination findings, and the nature of the planned surgical procedure. Routine testing isn’t universally mandated for healthy patients undergoing minor surgery; however, a baseline assessment is often prudent.
Commonly ordered tests include a complete blood count (CBC) to assess for anemia or infection, electrolytes to evaluate fluid and electrolyte balance, renal function tests (BUN, creatinine) to assess kidney function, and coagulation studies (PT, aPTT) to identify bleeding disorders.
For patients with significant comorbidities – cardiac, pulmonary, renal disease – or undergoing major surgery, additional investigations may be necessary. These could include an electrocardiogram (ECG) to assess cardiac rhythm, chest X-ray to evaluate pulmonary status, and arterial blood gas (ABG) analysis to assess oxygenation and ventilation.
Interpreting these results in conjunction with the clinical assessment is crucial for optimizing the patient’s condition and minimizing anesthetic risks.
Airway Assessment and Management Planning
Airway assessment is paramount before any anesthetic procedure, predicting potential intubation difficulties is crucial for patient safety. This involves evaluating Mallampati score, thyromental distance, neck mobility, and history of obstructive sleep apnea or prior difficult intubation.
A thorough assessment guides the selection of appropriate airway management tools and strategies. For anticipated difficult airways, a difficult airway cart containing alternative devices – laryngeal mask airways (LMAs), fiberoptic bronchoscope, video laryngoscope – should be readily available.
A clear plan for both routine and emergency airway management must be established. This includes consideration of awake intubation, rapid sequence induction, and surgical airway access if necessary.
Documenting the airway assessment and management plan in the patient’s chart ensures effective communication among the anesthesia team and facilitates a smooth and safe airway management process.
III. Anesthetic Techniques
Anesthetic techniques encompass general, regional, and intravenous induction methods. Intravenous induction, a standard practice, involves stages of altered consciousness, relaxation, and surgical anesthesia.
General Anesthesia – Overview
General anesthesia induces a reversible loss of consciousness, providing analgesia and muscle relaxation essential for many surgical procedures. The process typically begins with intravenous induction, progressing through distinct stages – initial altered consciousness, a brief period of excitation, and ultimately, a state of surgical anesthesia characterized by profound muscle relaxation and suppressed protective reflexes, including respiration.
Careful monitoring is paramount during general anesthesia. Maintaining a stable core temperature, ideally between 36-37°C, is strongly recommended for cases lasting 30 minutes or longer, utilizing active warming systems and ambient temperature control when necessary; Simultaneously, comprehensive intraoperative monitoring, encompassing cardiovascular parameters like ECG and blood pressure, alongside respiratory metrics such as capnography and pulse oximetry, is crucial for detecting and addressing any physiological derangements promptly.
The Guidelines to the Practice of Anesthesia, revised by the Canadian Anesthesiologists’ Society (CAS), provide detailed guidance on administering and managing general anesthesia, emphasizing adherence to standardized protocols and best practices to ensure patient safety and optimal outcomes. These guidelines, available in both print and interactive eBook formats, serve as an invaluable resource for anesthesiologists, residents, and Certified Registered Nurse Anesthetists (CRNAs).
Regional Anesthesia – Overview
Regional anesthesia encompasses a variety of techniques – including neuraxial blocks (spinal and epidural) and peripheral nerve blocks – that provide analgesia and anesthesia to a specific region of the body by interrupting nerve conduction. This approach offers advantages such as reduced systemic effects compared to general anesthesia and potentially improved postoperative pain control.
Similar to general anesthesia, meticulous monitoring is essential during regional anesthesia. Core temperature management is strongly recommended for procedures lasting 30 minutes or longer, employing active warming strategies to prevent hypothermia. Cardiovascular and respiratory monitoring, utilizing ECG, blood pressure, capnography, and pulse oximetry, are crucial for detecting and managing potential complications like hypotension or respiratory depression.
The Guidelines to the Practice of Anesthesia, developed by the Canadian Anesthesiologists’ Society (CAS), offer comprehensive guidance on the safe and effective administration of regional anesthesia techniques. These guidelines, accessible through print and interactive eBook formats, emphasize proper patient selection, technique execution, and post-operative monitoring to optimize patient outcomes and minimize risks. Adherence to these standardized protocols is paramount for all practitioners.
Intravenous Induction of Anesthesia
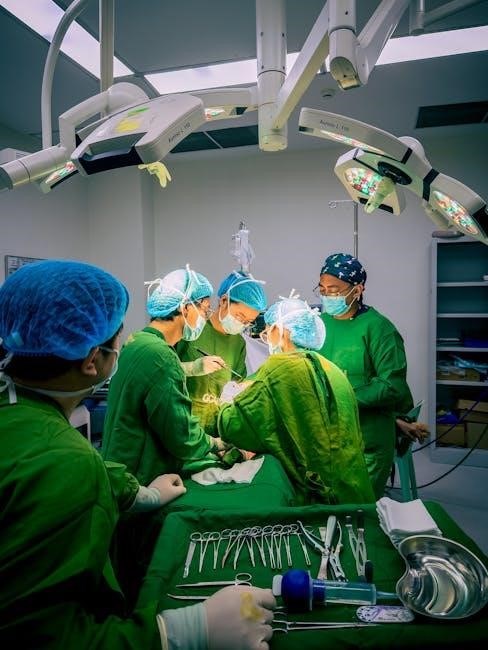
Intravenous induction is the predominant method for initiating general anesthesia in most surgical procedures. This process involves administering anesthetic drugs intravenously to rapidly induce a state of unconsciousness, allowing for subsequent airway management and maintenance of anesthesia. The induction phase progresses through distinct stages, characterized by altered consciousness, varying depths of anesthesia, and differing speeds depending on the chosen technique.
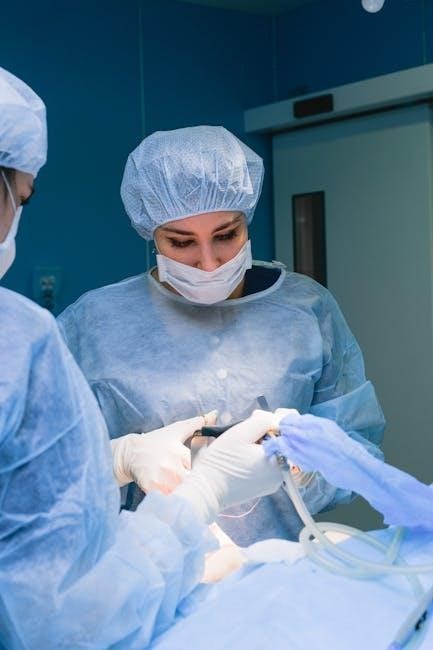
Typically, following anesthetic administration, patients experience a brief period of relaxation and disinhibition, often followed by a short phase of excitation before reaching the stage of surgical anesthesia. This stage is defined by muscle relaxation and a reduction or cessation of spontaneous breathing, necessitating ventilatory support.
The Guidelines to the Practice of Anesthesia, revised by the Canadian Anesthesiologists’ Society (CAS), provide detailed guidance on appropriate drug selection, dosing, and management of potential complications during intravenous induction. These guidelines, available in both print and interactive eBook formats, are essential resources for anesthesiologists, residents, and CRNAs striving to deliver safe and effective anesthetic care.
IV. Intraoperative Monitoring
Intraoperative monitoring, including core temperature, cardiovascular parameters (ECG, blood pressure), and respiratory function (capnography, pulse oximetry), is vital for patient safety.
Core Temperature Monitoring and Management
Core temperature monitoring is strongly recommended during surgical cases utilizing general or neuraxial regional anesthesia lasting 30 minutes or longer. Maintaining normothermia is a critical component of comprehensive patient care during anesthesia.
In the absence of specific surgical or patient-related indications necessitating intraoperative hypothermia, proactive measures should be implemented to actively warm the patient. These strategies include utilizing active patient warming systems, carefully controlling the operating room’s ambient temperature, and employing other appropriate techniques.
The primary goal of these interventions is to achieve and maintain a stable central core temperature within the target range of 36 to 37 degrees Celsius. Consistent monitoring allows for timely adjustments to warming strategies, preventing both hypothermia and hyperthermia, both of which can negatively impact patient outcomes.
Effective temperature management contributes to improved patient comfort, reduced risk of complications, and optimized physiological function throughout the surgical procedure and into the postoperative period.
Cardiovascular Monitoring (ECG, Blood Pressure, etc.)
Comprehensive cardiovascular monitoring is paramount during anesthesia administration, providing crucial insights into a patient’s hemodynamic status. Essential components include continuous electrocardiography (ECG) for arrhythmia detection and ST-segment analysis, alongside frequent and accurate blood pressure measurements—both non-invasive and, when indicated, invasive arterial pressure monitoring.
These measurements allow anesthesiologists to assess cardiac output, systemic vascular resistance, and overall perfusion. Pulse oximetry, while primarily respiratory, contributes to cardiovascular assessment by indicating oxygen delivery effectiveness. Vigilant monitoring enables prompt identification of hypotension, hypertension, or other cardiovascular instability.
The Guidelines to the Practice of Anesthesia emphasize the importance of individualized monitoring plans based on patient factors and surgical demands. Timely intervention, guided by these monitoring parameters, is essential for maintaining hemodynamic stability and preventing adverse events.
Continuous assessment and proactive management of cardiovascular function are fundamental to safe anesthetic practice.
Respiratory Monitoring (Capnography, Pulse Oximetry)
Robust respiratory monitoring is indispensable during anesthesia, ensuring adequate ventilation and oxygenation. Pulse oximetry provides continuous, non-invasive assessment of arterial oxygen saturation (SpO2), serving as a critical early warning system for hypoxemia. However, it’s crucial to remember pulse oximetry isn’t foolproof and can be affected by various factors.
Capnography, measuring end-tidal carbon dioxide (EtCO2), offers a more comprehensive evaluation of ventilation, detecting hypoventilation, rebreathing, and equipment malfunctions. It provides insight into the effectiveness of breathing and circulation. The Guidelines to the Practice of Anesthesia highlight capnography’s importance, particularly during procedures with potential for respiratory compromise.
Integrating both pulse oximetry and capnography provides a synergistic approach to respiratory monitoring. Regular assessment of respiratory rate, tidal volume, and auscultation further contribute to a complete picture. Proactive intervention based on these parameters is vital for preventing respiratory complications.
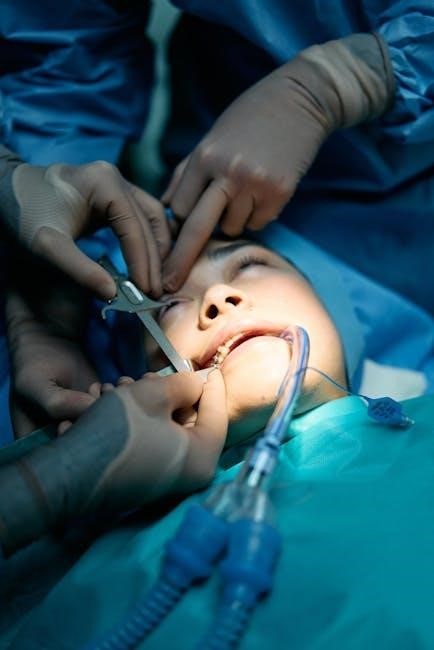
V. Patient Positioning and Safety
Patient positioning during anesthesia demands a team approach with meticulous attention to detail. Preventing pressure injuries and considering neurological implications are paramount for patient safety.
Preventing Pressure Injuries During Positioning
Pressure injuries represent a significant concern during surgical procedures requiring anesthesia, stemming from prolonged compression of skin and underlying tissues against bony prominences. A proactive, multidisciplinary approach is essential for prevention, involving careful patient assessment, strategic positioning, and diligent skin care.
The operating room team shares responsibility for identifying at-risk patients – those with pre-existing conditions like malnutrition, impaired perfusion, or fragile skin. Padding vulnerable areas, such as heels, elbows, sacrum, and occiput, with specialized pressure-redistributing devices is crucial.
Regular repositioning, ideally every two hours, or more frequently as clinically indicated, alleviates pressure and promotes tissue perfusion. Avoiding excessive force during positioning minimizes shear and friction, further reducing injury risk. Meticulous skin inspection throughout the procedure allows for early detection of any developing abnormalities.
Documentation of positioning strategies and skin assessments is vital for continuity of care and legal protection. Implementing standardized protocols and providing ongoing education to all personnel involved in patient positioning reinforces best practices and minimizes the incidence of pressure injuries.
Neurological Considerations in Patient Positioning
Patient positioning during anesthesia demands careful neurological assessment to prevent complications impacting the nervous system. Prolonged compression or stretching of peripheral nerves can lead to transient or, rarely, permanent nerve injury, manifesting as weakness, numbness, or pain.
Specific positions pose unique neurological risks. The lithotomy position, commonly used in gynecological and urological procedures, can compromise femoral nerve and sciatic nerve function if legs are improperly supported. Prone positioning, utilized for spine surgery, requires meticulous attention to head and neck alignment to avoid brachial plexus injury or ocular compromise.
Maintaining neutral alignment whenever possible minimizes nerve strain. Avoiding extreme joint angles and ensuring adequate padding are crucial. Careful monitoring of somatosensory evoked potentials (SSEPs) and electromyography (EMG) can detect early signs of nerve compromise during lengthy procedures.
Pre-existing neurological conditions, such as spinal stenosis or peripheral neuropathy, increase vulnerability. Thorough patient history and neurological examination are essential for tailoring positioning strategies and mitigating potential risks. Prompt recognition and management of any neurological deficits are paramount.
VI. Post-Anesthetic Care
Post-anesthetic care focuses on safe emergence, vigilant monitoring, and effective pain management protocols. Guidelines emphasize a smooth recovery, addressing potential complications promptly and efficiently.
Emergence from Anesthesia
Emergence from anesthesia is a dynamic process requiring careful observation and management. It involves the gradual return of consciousness, respiratory drive, and neuromuscular function following the discontinuation of anesthetic agents. The stages typically progress from initial responsiveness to full orientation, though individual experiences can vary significantly.
Monitoring vital signs – including heart rate, blood pressure, respiratory rate, and oxygen saturation – is paramount during emergence. Ensuring adequate airway patency and ventilation is crucial, potentially requiring assisted ventilation or airway adjuncts. Addressing post-operative nausea and vomiting (PONV) proactively is also essential for patient comfort.
Clinicians must assess the patient’s level of pain and provide appropriate analgesia according to established pain management protocols. A calm and reassuring environment can facilitate a smoother emergence, minimizing anxiety and agitation. The Guidelines to the Practice of Anesthesia Revised Edition 2025 emphasizes a structured approach to emergence, prioritizing patient safety and well-being throughout the recovery phase. Careful documentation of the emergence process is also vital for continuity of care.
Pain Management Protocols
Effective pain management is a cornerstone of post-anesthetic care, significantly impacting patient recovery and satisfaction. Protocols should be multimodal, integrating pharmacological and non-pharmacological approaches to address acute post-operative pain. Opioids remain a frequent component, but their use must be balanced with strategies to minimize side effects like nausea, respiratory depression, and constipation.
Non-opioid analgesics, such as acetaminophen and NSAIDs, play a crucial role in reducing opioid consumption and enhancing pain control. Regional anesthesia techniques, when appropriate, can provide prolonged analgesia with minimal systemic effects. The Guidelines to the Practice of Anesthesia Revised Edition 2025 advocates for individualized pain management plans tailored to the patient’s surgical procedure, pain intensity, and medical history.
Regular pain assessment using validated scales is essential for guiding treatment adjustments. Patient education regarding pain management options and potential side effects empowers them to actively participate in their care. Proactive pain control, rather than reactive treatment, is the preferred approach, aiming to prevent pain escalation and improve overall outcomes.